The Gut-Brain Connection
Understanding how the nervous system can influence digestion when answers aren’t clear

When the Tests Are Normal, But the Symptoms Are Not
Many people dealing with ongoing digestive issues eventually find themselves in the same place. They’ve seen doctors, run tests, and tried different diets, yet nothing fully explains what’s going on. Sometimes everything comes back “normal,” but the symptoms clearly don’t feel normal.
They’re disruptive, unpredictable, and often frustrating to live with day to day. Over time, it can start to feel like you’re just managing something no one can quite define.
So the question naturally becomes: if nothing is showing up on tests, what is actually driving this?
One possible explanation lies in the connection between the gut and the nervous system.
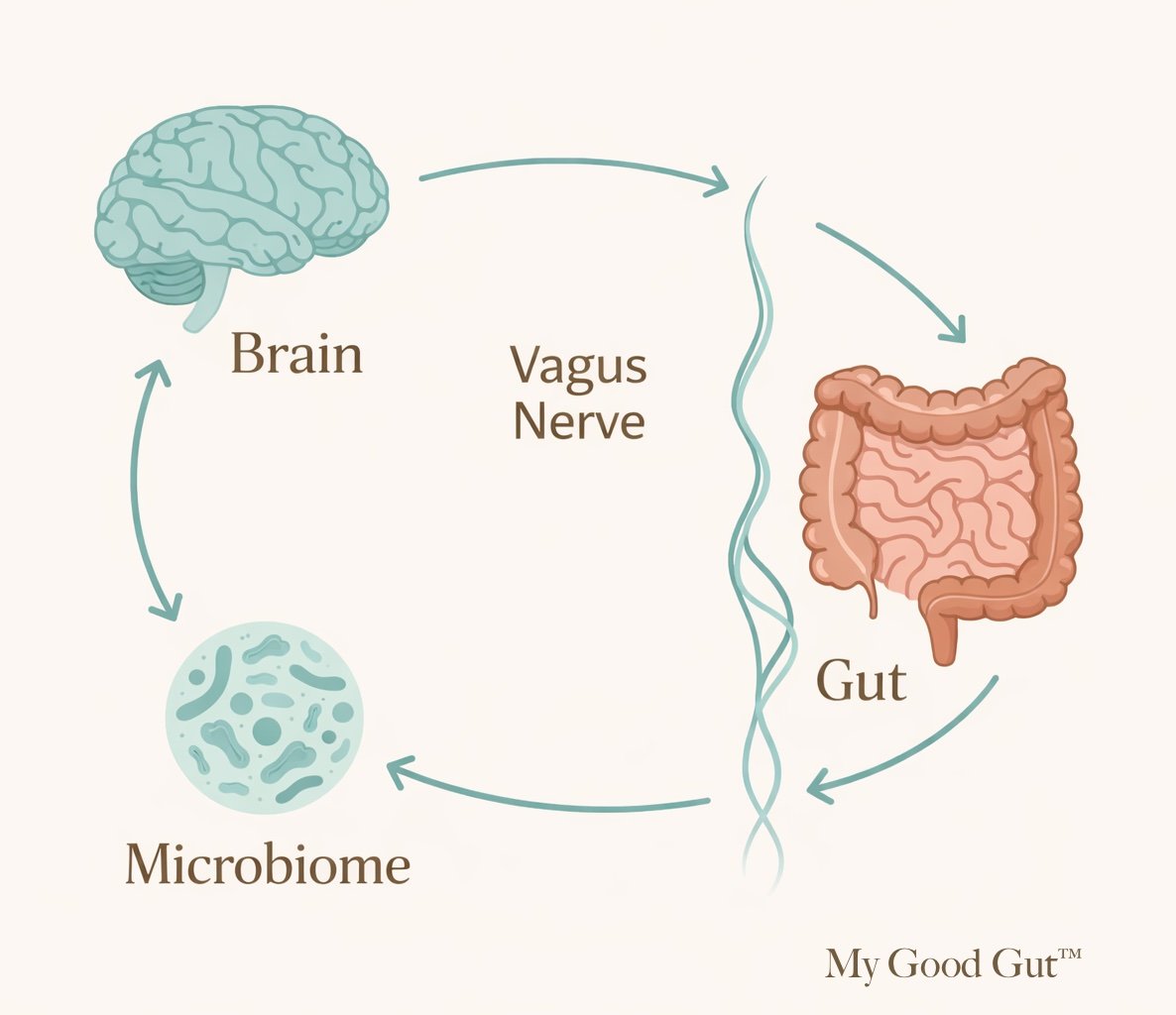
Your digestive system isn’t operating in isolation. It’s in constant communication with your brain through nerves, hormones, immune signals, and even the microbiome. Because of that, digestion is influenced not only by what you eat, but also by how your body is processing internal signals, stress, and sensation.
When that communication becomes dysregulated, normal digestive activity can start to feel anything but normal. Bloating, urgency, discomfort, and pain can show up even when there’s no clear structural issue.
This is why modern gastroenterology uses the term Disorders of Gut–Brain Interaction. It doesn’t suggest that symptoms are imagined. It points to the idea that the system controlling digestion may not be functioning in a balanced way.
For people who have already gone through the medical route without clear answers, this perspective can open up a different way of understanding what’s happening.
Q: Why do digestive symptoms continue even when tests are normal?
Answer: In some cases, the issue isn’t structural but functional. The digestive system may be physically intact, but the signaling between the brain and gut is out of sync. When that communication becomes overly sensitive or reactive, normal digestive activity can be experienced as discomfort, urgency, or pain.
The Gut–Brain Spectrum
Not all digestive issues come from the same source. Some are clearly tied to identifiable medical conditions, while others involve food sensitivities or microbiome imbalance. There is also a group of people whose symptoms appear to be more closely linked to how the nervous system is interacting with the gut.
It can be helpful to think of this as a spectrum.
Mostly Physical
Structural conditions, inflammation, infection
Mixed
Combo of physical triggers and nervous system sensitivity
Mostly Gut–Brain
Patterns in communication between the brain and gut
All three positions are valid, and all three can produce very real physical symptoms.
For individuals who have had extensive testing without clear findings, it is reasonable to consider that the nervous system may be playing a more central role than originally assumed.
Q: Can the nervous system really affect digestion that much?
Answer: Yes. The nervous system directly influences how the digestive tract moves, how sensitive it is to normal activity, and how signals are interpreted. When the body is in a more activated state, the gut can become more reactive, even in the absence of a clear physical trigger.
The Vagus Nerve
A key part of the gut–brain connection is the vagus nerve. It acts as a communication pathway between the brain and many organs, including the digestive system.
When vagal activity is strong and balanced, the body is more likely to be in a calm, regulated state where digestion can function smoothly. When that signaling is reduced, the body tends to stay in a more activated state, which can interfere with digestion.
While you can’t control the vagus nerve directly, you can influence it through certain patterns, especially breathing, relaxation, and attention.
Why the Nervous System Matters
The body is constantly evaluating whether it is in a state of safety or stress. That internal state directly affects how digestion works.
When the body shifts into a more alert or stressed state, digestion is no longer the priority. Motility can change, sensitivity can increase, and normal sensations can start to feel more intense or uncomfortable.
Over time, this pattern can become reinforced. The digestive system begins reacting more quickly and more strongly, even when there is no immediate reason for it to do so.
This doesn’t mean something is broken. It suggests the system may be over-responsive, and that over-responsiveness can often be retrained.
This is where things often become more actionable. Being told to “reduce stress” is vague and not particularly helpful. The nervous system responds better to specific, repeatable inputs. The following practices are simple, but they are directly connected to how the gut–brain system operates.
Practical Gut–Brain Practices

This is one of the most commonly used techniques in gut-focused programs.
Sit comfortably with one hand resting on your abdomen. Breathe in slowly through your nose and allow your belly to expand, then exhale slowly and let it soften. The goal is not to take exaggerated breaths, but to create a steady, relaxed rhythm.
Practiced consistently, this can help shift the body toward a more settled state that supports digestion.
Diaphragmatic Breathing

What you do right after eating can influence how your body processes that meal.
Instead of immediately returning to work, screens, or activity, take a few minutes to slow down. Sit, breathe, and allow your body to stay relatively still for five to ten minutes.
This gives your system a clearer signal that it can focus on digestion.
Post-Meal Reset

If you’ve dealt with symptoms for a long time, it’s natural to monitor your gut closely. The challenge is that constant monitoring can make sensations feel more intense.
A helpful shift is to practice noticing sensations without immediately reacting to them. Sit quietly, bring your attention to your abdomen, and observe what you feel without trying to change it.
Over time, this can reduce the automatic “something is wrong” response that tends to amplify symptoms.
Noticing Without Reacting

You can combine these elements into a short daily routine.
Start by sitting comfortably with your feet on the floor and one hand on your abdomen. Spend a couple of minutes breathing slowly, allowing your belly to rise and fall naturally. Then bring in a simple visualization, imagining your digestion moving in a smooth, steady rhythm. For the final minute, repeat a calming phrase to yourself, such as “my body can find balance.”
The goal is not immediate results. What matters more is consistency and repetition over time.
5-Minute Reset
Q: What is gut-directed hypnotherapy and how does it work?
Answer: Gut-directed hypnotherapy uses guided relaxation and focused imagery to help regulate communication between the brain and digestive system. Over time, this can reduce sensitivity, improve coordination of digestive processes, and help shift the system out of reactive patterns.
Gut-Directed Hypnotherapy
Gut-directed hypnotherapy is one of the more studied approaches for conditions like Irritable Bowel Syndrome.
Despite the name, it’s not about losing control or being put into a trance. It’s a structured way of using relaxation and guided imagery to influence how the brain and digestive system communicate.
Sessions typically involve calming the body, focusing attention inward, and visualizing smooth, coordinated digestive function. The intention is to reduce sensitivity and help the system move out of reactive patterns.

Self-Guided Gut Hypnotherapy Exercise
(Note: this is an exercise designed to help you go deeper than breathing or short resets practices.
It is best done in a quiet setting where you won’t be interrupted)
Sit or lie down comfortably and allow your body to settle. Close your eyes and begin with a few slow, steady breaths, letting your body relax naturally without forcing it.
After a minute or two, bring your attention to your abdomen. Instead of just noticing sensations, begin to actively guide your attention.
Imagine your digestive system as a coordinated, rhythmic system. You might picture gentle waves moving through the intestines, or a smooth, steady flow that moves without resistance.
Now, begin to layer in suggestion. Silently say to yourself, in a calm and matter-of-fact way:
“My digestion is steady and coordinated.”
“My system knows how to regulate itself.”
“There is no need for urgency or overreaction.”
Let these statements feel neutral rather than forced. The goal is not to convince yourself of something dramatic, but to introduce a different signal.
As you stay with the visualization, imagine any areas of tension in the gut gradually softening. Picture movement becoming more even, less reactive, more predictable. If your mind drifts, gently bring it back to the image and the rhythm.
Spend about 10 minutes here if you can. When you’re ready to finish, slowly bring your awareness back to your body and open your eyes.
*Repeating this exercise daily (or frequently as possible) is what helps re-train the communication between the brain and the digestive system over time.

When to Consider Working with a Hypnotherapist
If you’ve explored the practices on this page and want to go deeper, working with a trained hypnotherapist who specializes in digestive health can be a next step.
Gut-directed hypnotherapy is typically done over a series of sessions and focuses on helping the brain and digestive system communicate in a more regulated way. Unlike general hypnotherapy, this approach is tailored specifically to digestive symptoms and gut–brain patterns.
When looking for a practitioner, it’s important to find someone who has experience with IBS, digestive conditions, or gut-directed hypnotherapy specifically.
If you’re not sure where to start, you can use our Gut Health Concierge™ to help you find options in your area. The Concierge can:
Help you search for hypnotherapists near you
Identify practitioners who mention digestive or gut-related work
Suggest questions you may want to ask before booking a session
This can make the process more straightforward, especially if you’re not sure what to look for.
Digestive Health Hypnotherapy App
If you prefer a self-paced approach rather than working directly with a hypnotherapist, you may want to explore Nerva.
Nerva is a structured, gut-directed hypnotherapy app designed specifically for digestive health. It delivers guided audio sessions over a series of weeks, using techniques similar to those used in clinical gut-directed hypnotherapy programs.
Because it’s self-paced, it can be a more flexible option for those who prefer to work through the process on their own or want to explore this approach before committing to working with a practitioner.
