
LIMITED-TIME PREVIEW ACCESS
GLP-1 Medications
& Gut Health
Understanding Digestion Before, During, and After GLP-1 Use
GLP-1 medications are increasingly prescribed for weight management and metabolic conditions. Much of the public discussion focuses on appetite regulation, blood sugar, and weight change, while less attention is given to their effects on the digestive system.
For many individuals, some of the most noticeable effects of GLP-1 medications involve digestion. This page is intended to explore those changes and provide educational insights related to digestive comfort across different phases of GLP-1 use.

How To Support Your Gut on GLP-1
Preparing Your Gut Before Starting GLP-1
Beginning a GLP-1 medication can alter appetite, gastric emptying, and bowel patterns. Taking time to strengthen general digestive habits beforehand may improve overall comfort as your body adjusts.
Consider focusing on foundational digestive stability prior to starting:
Paying attention to ongoing symptoms such as bloating, irregular bowel patterns, or reflux and discussing concerns with your healthcare provider
Reducing ultra-processed foods, refined sugars, excess alcohol, and heavily refined oils
Gradually introducing soluble fiber from well-tolerated sources
Maintaining consistent hydration and electrolyte intake
Making dietary adjustments gradually rather than all at once
Preparation is not about perfection. It’s about creating steadier baseline habits so digestive changes feel more manageable.

Maintaining Your Gut While Taking GLP-1
While taking a GLP-1 medication, digestion may feel slower or more sensitive. Appetite patterns often shift, which can influence food variety, fiber intake, and hydration.
Paying attention to digestive patterns during this phase can help maintain comfort and consistency.
Common considerations people explore include:
Eating smaller portions and taking time with meals
Focusing on nutrient-dense, well-tolerated foods
Keeping fiber intake steady rather than increasing abruptly
Monitoring bowel regularity and discussing persistent constipation with a healthcare provider
Choosing foods that feel gentle and supportive
Observing symptom trends instead of reacting to single episodes
The aim is not to return digestion to its prior rhythm, but to understand and adapt to how it functions during GLP-1 use.
Caring For Your Gut When Coming Off GLP-1
After discontinuing a GLP-1 medication, appetite and digestive patterns may shift again. Hunger cues often return quickly, while gastric motility and bowel rhythm can take time to recalibrate. During this period, digestion may feel inconsistent or more reactive than expected.
Maintaining awareness during this transition can help create steadier adjustment.
Common considerations people explore include:
Gradually increasing portion sizes rather than returning abruptly to previous habits
Re-establishing consistent meal timing and food variety
Choosing balanced, well-tolerated meals
Paying attention to changes in bowel patterns or reflux
Monitoring symptom trends and discussing persistent concerns with a healthcare provider
Coming off GLP-1 is typically another phase of digestive adaptation. Observing patterns and making gradual adjustments may feel more sustainable than rushing back to prior routines.
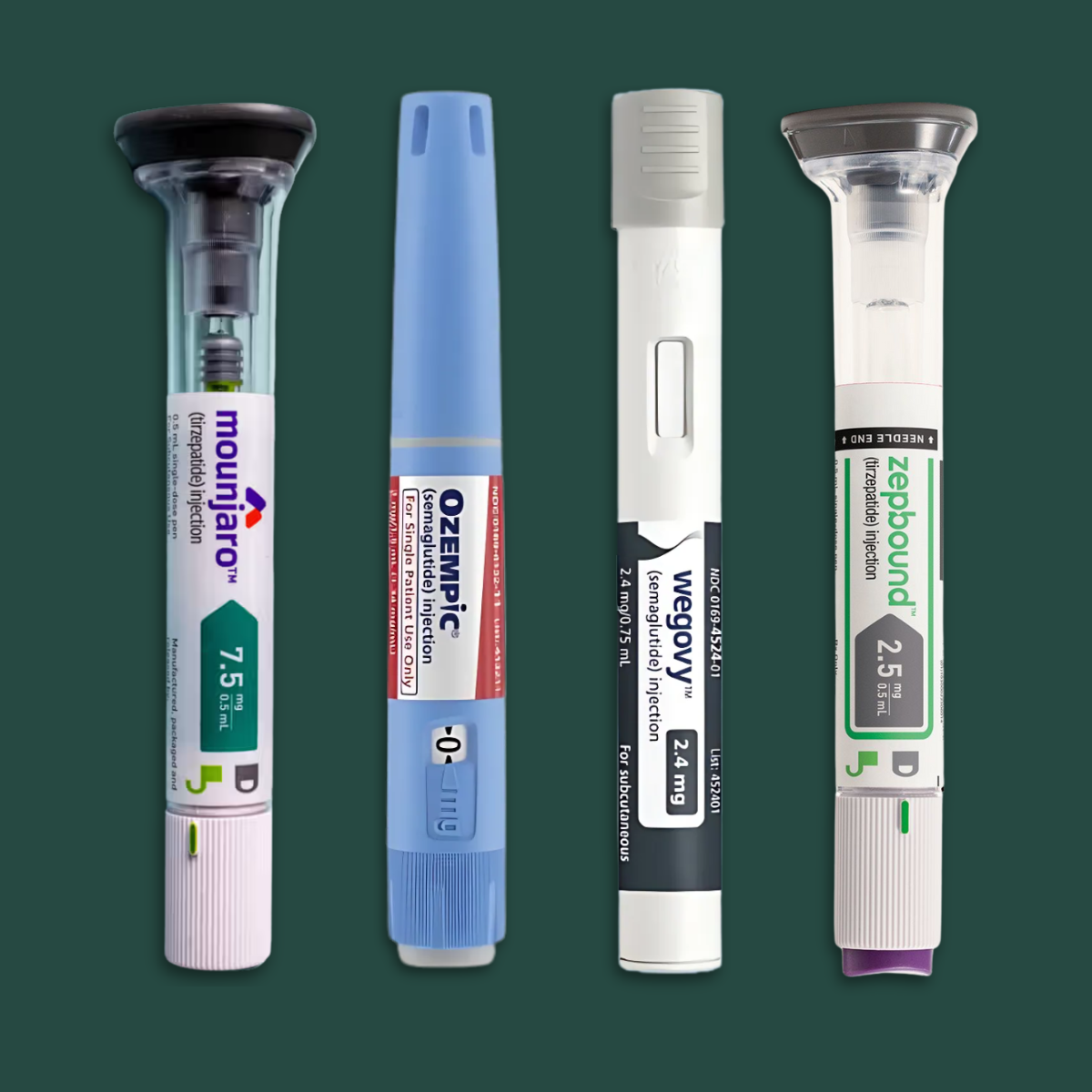
Understanding GLP-1 Medications
GLP-1 medications work by mimicking natural hormones involved in appetite regulation, gastric emptying, and blood sugar control. While several options are available, they share similar effects on digestion and motility.
Common GLP-1 options include:
Ozempic® (semaglutide) — a weekly injectable approved for type 2 diabetes that also affects appetite and digestion
Wegovy® (semaglutide) — a weekly injectable approved for chronic weight management
Mounjaro® / Zepbound® (tirzepatide) — dual-action medications affecting GLP-1 and GIP pathways
Rybelsus® (oral semaglutide) — a daily oral formulation targeting the same GLP-1 pathway
All GLP-1 medications influence digestive function, though individual responses vary. This page does not recommend one medication over another. Its purpose is to provide general educational context about digestive considerations that may arise during GLP-1 use.
Accessing GLP-1 Medications Through Telehealth
GLP-1 medications require evaluation and prescription by a licensed healthcare provider. Good Gut Goodies does not prescribe medications and does not sell pharmaceutical products. For individuals who do not already have a prescribing provider, telehealth services may offer a convenient way to explore eligibility and receive medical oversight. Availability, pricing, and access vary by individual, state regulations, insurance coverage, and medication supply.
Below are two national telehealth platforms operating within the United States:
Ro — connects individuals with U.S.-licensed clinicians who assess eligibility for GLP-1 medications and manage prescriptions when appropriate. Listing does not imply endorsement.
WeightWatchers — offers a structured medical and lifestyle program that includes telehealth-based GLP-1 prescribing along with nutrition and behavioral support.
Disclosure: My Good Gut participates in the WeightWatchers affiliate program and may earn a commission if you enroll through our link, at no additional cost to you. Individuals should consult their own healthcare provider when making decisions about prescription medications.
